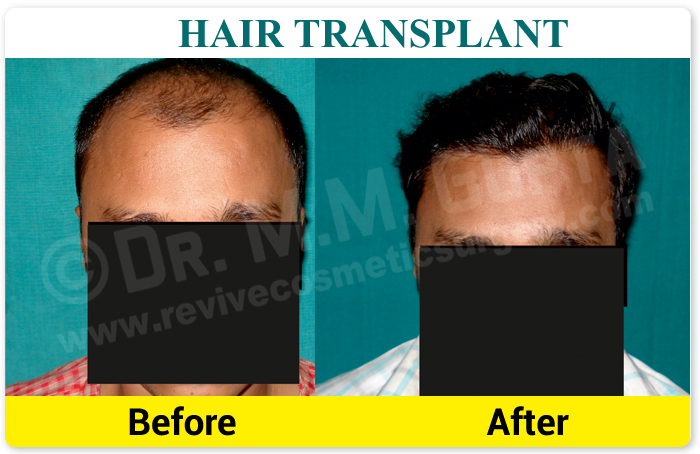
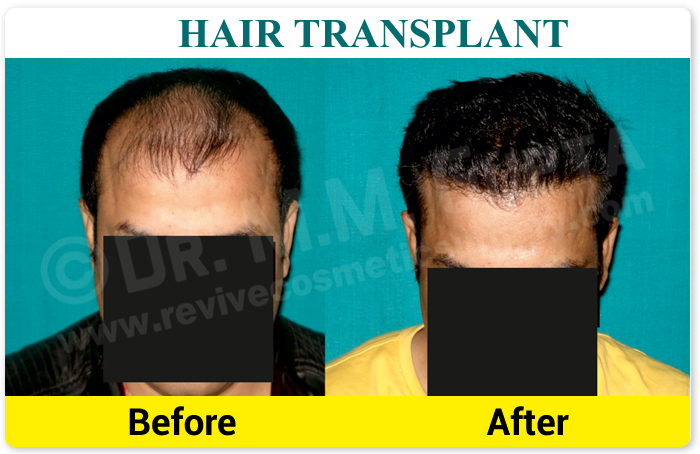
- Pioneer of Hair Transplant with world's latest & Best Technique FUT, in up
- Excellent Quality Hair Transplantation by highly Skilled & Experienced Plastic Surgeon
- Pioneer of Hair Transplant with scar less technique FUE, in up
- World class surgery at affordable cost with life changing results
- Pioneer of body hair to scalp transplant in up
- Many thousand patients with successful Hair Transplant results
Quick Contact
revivecliniclko@gmail.com
+91 9721476547, +91 8400746979

Female Genital Plastic Surgery

The procedures that comprise "Female Genital Plastic Surgery" include- Labiaplasty (Labia Minora Reduction), Labia Majoraplasty (Labia Majora Reduction, Labia Majora Augmentation) , Monsplasty (Mons Pubis Reduction), Vaginoplasty (Tightening of the vaginal wall, specifically at the entry point to the vagina), Clitoral Hood Reduction, and Hymenoplasty (Hymen Restoration).
Before discussing each one, it is important to look at the anatomy.
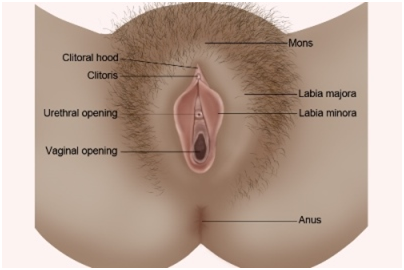
External anatomy of the female genitalia
The hair bearing area over the pubic bone at the upper portion of the female genitalia is called the mons. The hair-bearing outer lips are called the labia majora (singular is labium majus). The inner lips are called the labia minora (singular is labium minus). In the upper portion in the center is the clitoral hood, sometimes called the prepuce, which covers the clitoris in part or entirely. Below the clitoris is the urethral opening, and below that is the vaginal opening.
Hymenoplasty surgery
Hymenoplasty, also called Revirgination or Hymenorrhaphy, is a surgical procedure that uses a flap of vaginal lining to reconstruct a broken hymen or, in some cases, creates one for a woman who was born without. The procedure is typically performed in order to cause bleeding during post-nuptial intercourse, which in some cultures is considered proof of virginity.
Contrary to popular belief on this front, a hymen can rupture for any number of non-sexual reasons such as like
- horse-back riding
- gymnastics
- inserting of a tampon
- plus many more reasons
The term Hymenoplasty may cover at least three significantly different types of procedures -
- Suturing of a tear in the hymen such as might be caused by sexual assault, soon after the assault, to facilitate healing.
- A purely cosmetic procedure in which a membrane without blood supply is created, sometimes including a gelatin capsule of an artificial bloodlike substance. This operation is intended to be performed within a few days before an intended marriage.
- Use of a flap of the vaginal lining, complete with its blood supply, to create a new hymen. Patients are advised to refrain from penetrative sex for up to three months following this procedure.
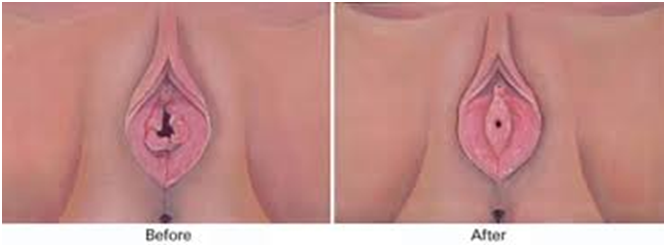
Typically, the procedure takes 1 to 2 hours and is performed under local anesthesia as a day care procedure. Some patients prefer the addition of IV sedation or even general anesthesia. Very fine invisible sutures are applied from the inside to repair torn hymen. These sutures automatically absorb itself within 2-3 weeks time. You will go home after surgery; there is no need for an overnight stay in the hospital.
Labiaplasty
The term labiaplasty refers to a procedure that reduces the length of the labia minora. Women opt for surgery for a variety of reasons, including pain from twisting
and tugging of the labia when riding a bike or during intercourse, itching, irritation and self-consciousness.
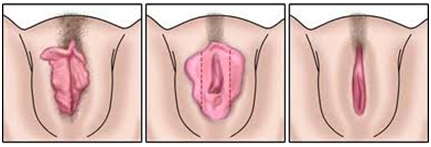
The goal of the procedure is to reduce the labia minora so that they don't hang below the hair-bearing labia majora. A labiaplasty may be performed to reduce asymmetry when one is longer than the other, or, more commonly, to reduce the length of both labia so that the labia no longer twist, tug or fall out of a bathing suit.Procedure
Relatively, the procedure is simple, excising an area of the labia minora using a variety of incisions and takes 1 to 2 hours and is performed under local anesthesia as a day care procedure. Some patients prefer the addition of IV sedation or even general anesthesia. You will go home after the surgery; there is no need for an overnight stay in the hospital. Careful placement of the scar is important, however, in order to prevent painful scar contracture along the rim of the labia.
Recovery
Most patients take a week off from work, during which they can reduce swelling and pain by icing with a cold pack. Patients can resume wearing tampons or having intercourse after four to six weeks. Trim labiaplasty generally allows for a quicker recovery. While the most distorting swelling is gone by 6 weeks, residual swelling may take six months to disappear.
Risks of a Labiaplasty
The risks associated with labiaplasty include those of most surgical procedures, including bleeding, hematoma and infection. The most common complication is over-resection. While some women desire an aggressive reduction, this can result in chronic dryness, scarring at or near the vaginal opening and pain with intercourse. Healing problems are more likely to occur with a wedge procedure, particularly if the patient is exposed to substances that cause blood vessels to shrink.
Labia Majoraplasty
A labia majoraplasty is a procedure designed to surgically reduce the size of the outer, hair-bearing labia majora. Patients who feel their labia majora are too large or hang down may feel discomfort from such activities as cycling, or they may be embarrassed by the fullness.
Procedure
This procedure can be done under local anesthesia with oral sedation or general anesthesia, depending on the amount of tissue to be removed. The plastic surgeon removes two slight crescents of skin from the inner portion of each labium. The amount to be removed depends on the amount of excess tissue. Closure is usually done with absorbable sutures.
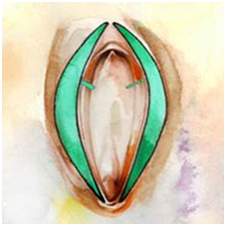
Risks of a labia majoraplasty
Risks include bleeding, hematoma, infection, scarring, under resection, over resection.
Recovery
Most patients take a week off from work, during which they can reduce swelling and pain by icing with a cold pack. Patients can resume wearing tampons or having intercourse after four to six weeks. Swelling after a labia majoraplasty can last 6 months or longer, depending on the thickness of the tissue, although much of the swelling is gone by 6 weeks.
Labia Majora Augmentation
In some women; with aging, after child birth, or with weight loss; the labia majora may undergo a significant atrophy and the dermis under the skin thins out. As a result of these changes the labia majora becomes shrunken, flat, saggy, wrinkled, and darkened. The surgeon can drastically augment and rejuvenate the labia majora with micro fat grafting.Procedure
The process requires gentle fat removal from areas such as the abdomen, flanks, hips or thighs using low-vacuum liposuction and the use of thin, delicate, non-traumatic cannulas to protect the survival of each harvested living fat cell. The fat cells are then purified and slowly injected through tiny skin incisions into the tissue of the recipient site utilizing a small syringe and cannula. Tiny droplets are placed throughout the tissues assuring that each transferred fat cell will have an adequate blood supply to achieve the permanent survival of the injected fat cells.
Clitoral Hood Reduction
Excess folds of the clitoral hood, or prepuce, can be reduced with a clitoral hood reduction. It leaves the highly enable surface of the clitoral node to be more exposed, resulting in increased female sexual orgasms. The extra folds can create a bulge that is exaggerated when the labia minora are reduced, and a clitoral hood reduction can improve the balance in appearance of the female genitalia. The procedure is more commonly done along with a Labiaplasty.
Procedure
A clitoral hood reduction is usually done under either local anesthesia with oral sedation or under general anesthesia. The excess tissue is marked according to the individual's anatomy. There is a wide variation in the shape and extent of folds. In some patients the excision is performed as a "Y" extension off the labiaplasty. Closure is usually done with absorbable sutures.

Monsplasty
A monsplasty is a procedure designed to reduce bulging of the mons, the upper part of the hair-bearing part of their vulva. The bulge can result in women feeling too embarrassed to wear a bathing suit or tight pants. The purpose of a monsplasty is to reduce the amount of fatty tissue and/or skin, depending on the cause of the bulge.
Procedure
Depending on the amount of tissue to be removed, local anesthesia with oral sedation may be used for some procedures, but general anesthesia may be preferable in others. Sometimes the amount of skin removed can be extensive, while in others, liposuction is sufficient.
Recovery
Recovery takes about a week, with physical activity restrictions for two to six weeks, depending on the extensiveness of the procedure. If skin is removed, a drain or two may be placed, with removal typically scheduled within the first few days.
Vaginoplasty
After childbirth, women may complain of vaginal laxity, resulting from stretching of tissues and separating of muscles, sometimes to the point that a tampon falls out, and this lack of tone can contribute to sexual dysfunction. Vaginoplasty (also known as Posterior Colporrhaphy) is a procedure designed to tighten the vagina. A vaginoplasty brings the separated muscles together, and the extra mucosa skin from the back side of the vagina is removed. The external skin can also be removed for a more aesthetic appearance. Vaginoplasty or Vaginorrhaphy tightens and restores the diameter of vagina and supporting structures to near "pre-pregnancy" state, thereby re-establishing friction that may increase sexual satisfaction for both women and men.
Vaginoplasty can also be performed as reconstructive procedure for correcting the defects and deformities of the vaginal canal and its mucous membrane, and of vulvo-vaginal structures that might be absent or damaged because of congenital disease (e.g. vaginal atresia) or because of an acquired cause (e.g. physical trauma, cancer). As such, the term vaginoplasty generally describes any such vaginal surgery, and the term neo vaginoplasty specifically describes the procedures of either partial or total construction or reconstruction of the vulvo-vaginal complex.
Procedure
Vaginoplasty can be done under local anesthesia; some opt to have it done under general anesthesia. Patients are asked to do bowel prep prior to surgery. The procedure may be as simple as placing sutures at the introitus (vaginal opening), or may involve excising excess vaginal mucosa together with tightening the muscles of the posterior vaginal wall. If there is external skin that protrudes, this can be reduced as well for a more aesthetic result. Neovaginoplasty may involve taking skin from your thigh & creating a new vagina through it.
Recovery
Patients may have one to two weeks of down time. They may feel a deep ache for the first few days, and there is no tampon use or intercourse for eight weeks. Depending on the amount of tightening performed, some patients may be instructed to use dilators.
What makes us unique?
Our Efficiency | Our Competency | Our Reliability | Our Dedication | Our Expertise in the respective fields.
Best Doctors
We have a team of doctors who are best in their respective fields of specialization for best results and maximum patient safety.
Best Plastic & Cosmetic Surgeon
MBBS, MS, MCh, DNB
- Our plastic and cosmetic surgeon are highly trained and best Hair Transplant Surgeon with more than 14 years of experience in doing Hair Transplant with excellent & world-class results.
- The most trusted, skilled, and experienced Hair Transplant and Cosmetic Surgeons in Lucknow and Varansi is owned by Revive Clinic
- Our surgeon is a Pioneer of the FUT technique of Hair Transplant in Uttar Pradesh.
- Our surgeon is a Pioneer of the FUE technique of Hair Transplant in Uttar Pradesh.
Best Gynecological Surgeon
MBBS, DGO, DNB
- Our gynecological and obstetrics doctor is highly trained Obstetrician, Gynecologist & Laparoscopic Surgeon with more than 17 years of experience.
- Our gynecological and obstetrics doctor is working as a Senior Consultant Obstetrician & Gynecologist at Fatima Hospital, Lucknow.
- Revive Clinic posseses one of the best and highly experienced Obstetrics & Gynecology & Laparoscopic doctors in Lucknow.
Ultra-modern Centre
Hair Transplant Center
- We have state of art ultra-modern facility for hair transplant. We use ultra-hygienic and the best safety method for patient care.
- We have a dedicated Hair Transplant Operation Theater (Hair Lab.) with temperature and humidity control, ergonomically designed cutting platform, cold lights, ceiling lights with heat filters, preventing any damage to the Hair grafts.
- Revive Clinic is one of the leading hair transplant clinics in Lucknow, Uttar Pradesh, India. Our hair treatment procedures are best in class and give the best results.
- We offer the best hair transplant treatment with all the latest and best techniques & instruments.
- We ensure maximum patient's privacy, it is our first priority.
Obstetrical & Gynecology Treatment
- We have advanced facilities & equipment for providing the best obstetrical & gynecological treatment.
- All treatments are done by our highly experienced doctor taking utmost care for giving the best results and high priority for patient safety.
- At Revive we evaluate every patient for normal delivery as a primary option, doctor opt for caesarian delivery only in high-risk conditions for the safety of mother and baby.
- Revive clinic is one of the best obstetrical & gynecological clinics in Lucknow.
- Revive Clinic offers a wide range of obstetrical & gynecological care i.e. From contraceptive counseling to general gynecological & obstetrical services including Infertility Treatment for women at different stages of life, we are best in our field.
Best Results
- Our success is well spoken by thousands of our happy and satisfied patients of Hair Transplant & Plastic & Cosmetic Procedures both national as well as international. We are committed to patient's safety & satisfaction.
- 100% natural-looking results are given by our best hair transplant and cosmetic surgeon, with no side effects.
- We provide the best hair transplant & cosmetic Surgery results at very affordable costs.
- We have excellent results for infertility treatment.
- We give the best results for all Obstetric & Gynecological problems at a very affordable cost.
Professional Staff
Why us

State of Art CenterLatest Equipment & Techniques
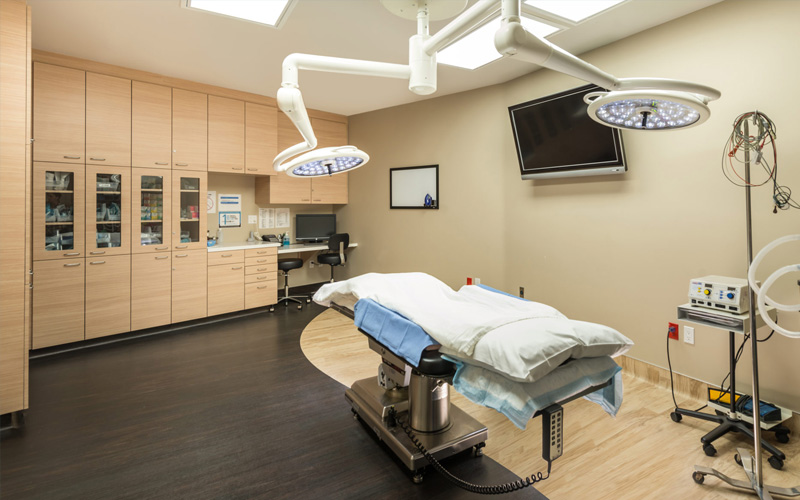
- We use latest Equipments & Techniques to deliver top class Treatments
- Our center have relaxing environment with modern facilities and look
Qualified Doctor & StaffBoard Certified and Specialized Team

- Dr. M. M. Gupta is; experienced, highly qualified and skilled cosmetic surgeon; providing surgical services of International Standard.
- Our team consists of trained and caring staffs, available 24x7 for patient's care.
World Class ResultsMaximum Patient Satisfaction

- Combination of State of Art Center and Experienced, Highly Qualified & Skilled Cosmetic Surgeon bring out world class results, every patient expect.
- You can see Live Surgical Procedures and also meet our satisfied clients to gain confidence about our Excellent Results.

Our Specialities

Quick Contact
revivecliniclko@gmail.com
+91 9721476547, +91 8400746979
Mail Your Query Here

Credentials
Face
Hair & Skin
Body
Breast